In a previous article in this series on diabesity and metabolic syndrome I briefly mentioned the role of gut health in obesity and diabetes. I’d like to go into more detail on that subject here, especially since it’s not a very well known relationship.
Our gut is home to approximately 100,000,000,000,000 (100 trillion) microorganisms. That’s such a big number our human brains can’t really comprehend it. One trillion dollar bills laid end-to-end would stretch from the earth to the sun – and back – with a lot of miles to spare. Do that 100 times and you start to get at least a vague idea of how much 100 trillion is.
The human gut contains 10 times more bacteria than all the human cells in the entire body, with over 400 known diverse bacterial species. In fact, you could say that we’re more bacterial than we are human. Think about that one for a minute.
We’ve only recently begun to understand the extent of the gut flora’s role in human health and disease. Among other things, the gut flora promotes normal gastrointestinal function, provides protection from infection, regulates metabolism and comprises more than 75% of our immune system. Dysregulated gut flora has been linked to diseases ranging from autism and depression to autoimmune conditions like Hashimoto’s, inflammatory bowel disease and type 1 diabetes.
Recent research has shown that the gut flora, and the health of the gut in general, also play a significant role in both obesity and diabetes. I’ve seen this anecdotally in my practice as well. Nearly every patient I treat with a blood sugar issue also has a leaky gut, a gut infection, or some other chronic inflammatory gut condition.
We now know that the composition of the organisms living in your gut determines – to some extent, at least – how your body stores the food you eat, how easy (or hard) it is for you to lose weight, and how well your metabolism functions. Let’s take a closer look at the mechanisms involved.
Intestinal Bacteria Drive Obesity and Metabolic Disease
A study published this year in Science magazine found that mice without a protein known as toll-like receptor 5 (TLR5) in their gut gain excessive weight and develop full-blown diabetes and fatty liver disease when fed a high-fat diet. If we think of the gut flora as a community, TLR5 is like a neighborhood police force that can keep the houligans in check. Without TLR5, bad bacteria can get out of control.
The study authors found that these bad bacteria caused a low-grade inflammation in the mice, which caused them to eat more and develop insulin resistance. They also found that treating these mice with strong antibiotics (enough to kill most of the bacteria in the gut) reduced their metabolic abnormalities.
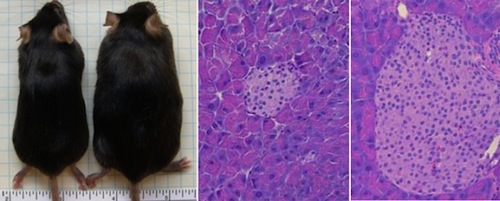
Other studies have shown that the composition of the gut flora differs in people who are obese and diabetic, and people who are normal weight with no metabolic irregularities.
One possible mechanism for how changes in the gut flora cause diabesity is that different species of bacteria seem to have different effects on appetite and metabolism. In the study on TLR5 deficient mice I mentioned above, the mice with too much bad bacteria in their guts experienced an increase in appetite and ate about 10 percent more food than their regular relatives. But it wasn’t just that these mice were hungrier and eating more; their metabolisms were damaged. When their food was restricted, they lost weight – but still had insulin resistance.
Other studies have shown that changes in the gut flora can increase the rate at which we absorb fatty acids and carbohydrates, and increase the storage of calories as fat. This means that someone with bad gut flora could eat the same amount of food as someone with a healthy gut, but extract more calories from it and gain more weight.
Bad bugs in the gut can even directly contribute to the metabolic syndrome by increasing the production of insulin (leading to insulin resistance), and by causing inflammation of the hypothalamus (leading to leptin resistance).
Like what you’re reading? Get my free newsletter, recipes, eBooks, product recommendations, and more!
How Modern Life Screws up Our Gut and Makes Us Fat and Diabetic
What all of this research suggests is that healthy gut bacteria is crucial to maintaining normal weight and metabolism. Unfortunately, several features of the modern lifestyle directly contribute to unhealthy gut flora:
- Antibiotics and other medications like birth control and NSAIDs
- Diets high in refined carbohydrates, sugar and processed foods
- Diets low in fermentable fibers
- Dietary toxins like wheat and industrial seed oils that cause leaky gut
- Chronic stress
- Chronic infections
We also know that infants that aren’t breastfed and are born to mothers with bad gut flora are more likely to develop unhealthy gut bacteria, and that these early differences in gut flora may predict overweight and obesity in the future.
It’s interesting to note that the diabesity epidemic has neatly coincided with the increasing prevalence of factors that disrupt the gut flora. I’m not suggesting that poor gut health is the single cause of obesity and diabetes, but I am suggesting that it likely plays a much larger role than most people think.
How to Maintain and Restore Healthy Gut Flora
The most obvious first step in maintaining a healthy gut is to avoid all of the things I listed above. But of course that’s not always possible, especially in the case of chronic stress and infections, and whether we were breastfed or our mothers had healthy guts.
If you’ve been exposed to some of these factors, there are still steps you can take to restore your gut flora:
- Remove all food toxins from your diet
- Eat plenty of fermentable fibers (starches like sweet potato, yam, yucca, etc.)
- Take a high-quality probiotic, or consider more radical methods of restoring healthy gut flora
- Treat any intestinal pathogens (such as parasites) that may be present
- Take steps to manage your stress
Better supplementation. Fewer supplements.
Close the nutrient gap to feel and perform your best.
A daily stack of supplements designed to meet your most critical needs.



Where you say
“Take a high-quality probiotic, or consider more radical methods of restoring healthy gut flora” the link leads to Bowel Disease, Part II: Healing the Gut By Eliminating Food Toxins
I wonder if you intended to link to go to Bowel Disease, Part IV: Restoring Healthful Gut Flora
It is more complicated than just replacing the gut flora. I had a colonoscopy earlier this year. I’d already switched to a primal diet a couple of months before the procedure and had my pro- and prebiotics ready for recolonization after the procedure. No real change in my health, still have high blood sugars etc.
Hans:
All of the toxins you mentioned play a significant role in dysregulating the gut flora, so yes, they have to be considered.
Nice HOT new topic. I wonder if the gut flora question can be seen without considering other gut undermining forces like gluten, lectins, saponins and glycoalkaloids. Very best regards, Hans
Solid science, Chris. Gut microbiota is strongly linked. Keep on getting the message out there. Let these fraud Internet gurus who push dieting hear you.
Obesity is extremely complex. There are vast unknowns and uncertainties. Real researchers already know this and admit it. My blog discusses a lot of the same thing . Obesity is only simple and certain to the $ 100 billion a year dieting industry which rests precariously on false assumptions and false promises .
Also ,please look into Urgelt from youtube. He says a lot of what you say too. That man is very intelligent and has a lot to say on obesity :))
Take care,
Razwell
I do recommend using a water filter. Chlorinated water can harm the gut flora.
Good posts!
What are your thoughts on drinking chemically treated municipal water? Does chlorine etc have an effect on gut flora? Should we be using appropriate filters? Or is this a non issue.
Thanks!
Also, Chris, do you agree with everything on those perfecthealthdiet.com links? Because some claims in them were reaallly not science-based, and I know you want to structure your posts according to the best evidence.
@Chris
We do have a progressive GP. Too bad the NHS isn’t as progressive. He’ll have to see a private doctor to see get something done about the problem.
Hi Chris,
Thanks for another excellent post. This is a subject that has fascinated me since it first came to my attention in your podcast interview with Dr. Guyenet. Since then I’ve been reading about the physiological role of fermentable fibers, and have found much scientific support for these ideas.
For example, check out this study, which found that an experimental group supplemented with resistant starch (a fermentable fiber) extracted from kidney beans lost more fat than a control group, even though both were fed a high-carb diet:
https://www.medsci.org/v04p0045.htm
Recently I began taking psylium husk supplements (1-2 grams) with each meal, and in the past two weeks I’ve averaged over a half-pound of weight loss per day, even though I’ve continued eating carb-heavy foods such fruit, orange juice, and brown rice and haven’t changed my exercise routine. Your readers might try this for themselves.
Hey Chris,
Since some of the studies you cited found bad effects on gut flora with a high fat diet, would you recommend a low-fat diet as a way to have healthy bacteria?
Hi Chris,
Love your article. One question, do I take probiotics forever or do we take it for a couple of years then give it a break and start again.
Thanks
Unfortunately, most of the highest quality brands aren’t available directly to consumers.
For brands you can buy in the store or online, I think Biokult (https://www.bio-kult.com/) is probably one of the best.
Prebiotics may ultimately be even more important than probiotics in restoring healthy gut flora, but some people don’t tolerate them well. They can cause a lot of gas and bloating, especially if you don’t build up the dose slowly.
Hey Chris, my company manufacturers an incredible digestion product that is single serve, powder, probiotic/prebiotic/enzymes. It has made a huge impact on our families health and that of many of my clients. My heart hurts for the mom suffering with her little 7 year old son. I would love to send her some samples with my compliments. It is not remotely about a “sale” for me, but the ability to help this child feel better and thrive. Any chance you can connect us? Thanks for your help!
Can u plz send info about your companys products? Tnx
Hi Phoebe, please send me information.
Hi Phoebe, I am interested too, any chance of sending your details trough to me please
Phoebe
You mentioned a prebiotic/priobiotic/enzyme that helps the good gut flora, on chriskresser web forum about healthy gut is key to hidden weight loss. Can you please provide me information and how to purchase it.
I am interested in the probiotic/prebiotic as well. Please send info to me as well if possible.
Thank you!
Chris, I was glad to see you also recommend PrescriptAssist soil based probiotic prebiotic. What are your thoughts on taking something like Biocult AND PrescriptAssist? (Starting with fractions of capsule and gradually increasing)
Chris – Any suggestions for high quality probiotics? And what do you think about prebiotics (e.g. fructooligosaccharides) as a potential supporter of gut health? Thanks!
The best choices are primarily starchy tubers like sweet potato, yam, yucca (a.k.a. manioc root), taro and lotus. White potatoes are also okay, but peeled since the skin has toxins and anti-nutrients.
hello. i was wondering if you could list some more fermentable starches. interesting topics dude. i would like to know some more of restoring gut health for my patients after antibiotic use for long term nsaid use.
Heather: absolutely. I’m amazed to hear a GP diagnose candida. You must have a very progressive GP!
I wonder if the same could be true for being underweight. My husband has a difficult time keeping weight on. I think he has some digestive issues. Recently his GP said that he might have a Candida problem. Could that be connected to his steady weight loss?
ahhh i love this article…now, if you could focus the big link between the brain-gut regulation i think you’d have a masterpiece…. a lot of what happens in the gut is a by product of the brain and vise versa…nice to see someone isnt focusing on calories and carbs 🙂
Excellent question.
The sequence goes like this: first remove, then replace, restore and repair.
It’s important to clear the infection first, because any attempts to repair the gut without doing that will otherwise be ineffective. Once the infection is cleared, the gut flora can be restored with probiotics and prebiotics, or fecal bacteriotherapy.
But there are more possibility for the removal of some good microbes with the worst one in the application of antibiotics. will not it hamper the natural microbiota?? And also when we restore the gut with external probiotics, the probability of these external agent’s to be dominated upon the natural microbiota will more!! Will not this be harmful??
Hi Chris,
How do you deal with the issue that the cure for chronic infections is antibiotics – which is also not good for your gut bacteria. At which point does the cure become worse than the disease its trying to combat?