This is the second article in a series on heartburn and GERD. If you haven’t read the first one, I’d suggest doing that first.
The idea that heartburn is caused by too much stomach acid is still popular in the media and the public. But as Daniel pointed out in the comments section of the last post, anyone familiar with the scientific literature could tell you that heartburn and GERD are not considered to be diseases of excess stomach acid.
Instead, the prevailing scientific theory is that GERD is caused by a dysfunction of the muscular valve (sphincter) that separates the lower end of the esophagus and the stomach. This is known as the lower esophageal valve, or LES. The LES normally opens wide to permit swallowed food and liquids to pass easily into the stomach. Except for belching, this is the only time the LES should open.
Here’s the key point. It doesn’t matter how much acid there is in the stomach. Even a small amount can cause serious damage. Unlike the stomach, the lining of the esophagus has no protection against acid.
Free eBook
Learn More about Heartburn and GERD
Download this free eBook to discover the little-known causes of heartburn and GERD, and find out how to get rid of the problem forever.
"*" indicates required fields
I hate spam, too. Your email is safe with me. By signing up, you agree to our privacy policy.
We’ve Been Asking the Wrong Question
In an editorial published in the journal Gastroenterology, the author remarked: (1)
Treating gastroesophageal reflux disease with profound acid inhibition will never be ideal because acid secretion is not the primary underlying defect.
I couldn’t agree more. For decades the medical establishment has been directing its attention at how to reduce stomach acid secretion in people suffering from heartburn and GERD, even though it’s well-known that these conditions are not caused by excess stomach acid. Instead, the question researchers should have been asking is, “what is causing the LES to malfunction?” Since it is universally agreed upon that this is the underlying mechanism producing the symptoms of GERD, wouldn’t it make sense to focus our efforts here? That’s exactly what we’re going to do in this article.
GERD Is Caused by Increased Intra-Abdominal Pressure
It is well accepted in the literature that GERD is caused by an increase in intra-abdominal pressure (IAP).
For example, several studies have indicated an association between obesity and GERD, and one paper in Gastroenterology concluded that increased intra-abdominal pressure was the causative mechanism. (2, 3) But while I agree that all of the currently accepted factors play a role, I do not think they are the primary causes of the increased IAP seen in GERD.
The Two Primary Causes of Increased Intra-Abdominal Pressure
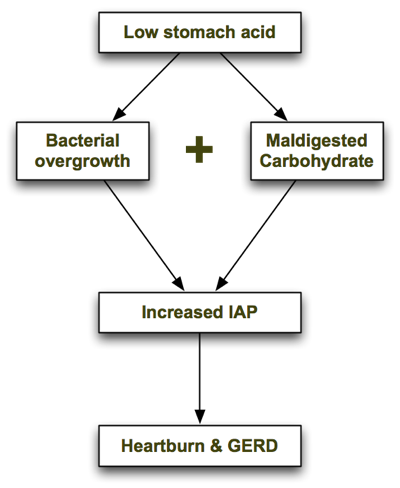
In his excellent book, Heartburn Cured, microbiologist Dr. Norm Robillard argues that carbohydrate malabsorption leads to bacterial overgrowth, resulting in IAP which drives reflux. Dr. Robillard makes a strong case that carbohydrate malabsorption plays a significant role in IAP, and I agree. But as I researched this issue I couldn’t help asking: what might be causing the carbohydrate malabsorption in the first place, and are there any other causes of bacterial overgrowth that may precede carbohydrate malabsorption? I believe the one answer to both of those questions is low stomach acid. Low stomach acid can contribute to both bacterial overgrowth (independently of carbohydrate intake) and carbohydrate malabsorption, as I describe below. In a nutshell, the process looks like this: Let’s look at each step in turn.
1. Low Stomach Acid Causes Bacterial Overgrowth
As I explain in the next article, one of the chief roles of stomach acid is to inhibit bacterial overgrowth. At a pH of 3 or less (the normal pH of the stomach), most bacteria can’t survive for more than 15 minutes. But when stomach acid is insufficient and the pH of the stomach rises above 5, bacteria begin to thrive. The gastrin knockout mouse, which is incapable of producing stomach acid, suffers from bacterial overgrowth—as well as inflammation, damage and precancerous polyps in its intestines. (4) It is also well documented that acid-suppressing drugs promote bacterial overgrowth. Long-term use of Prilosec, one of the most potent acid suppressing drugs, reduces the secretion of hydrochloric acid (HCL) in the stomach to near zero. In one trial, 30 people with GERD were treated with a high dose of Prilosec (40g/day) for at least 3 months. (5) Eleven of the 30 Prilosec-treated people had developed significant bacterial overgrowth, compared with only one of the 10 people in the control group.
2. Low Stomach Acid Causes Maldigestion of Carbohydrates
Stomach acid (HCL) supports the digestion and absorption of carbohydrates by stimulating the release of pancreatic enzymes into the small intestine. If the pH of the stomach is too high (due to insufficient stomach acid), the pancreatic enzymes will not be secreted and the carbohydrates will not be broken down properly.
Like what you’re reading? Get my free newsletter, recipes, eBooks, product recommendations, and more!
Bacterial Overgrowth + Maldigested Carbohydrates = GAS!
In Hearburn Cured, Dr. Robillard points out that though microbes are able to metabolize proteins and even fats, their preferred energy source is carbohydrate. The fermentation of carbohydrates that haven’t been digested properly produces gas. The resulting gas increases intra-abdominal pressure, which is the driving force behind acid reflux and GERD. From Dr. Robillard’s book:
According to Suarez and Levitt (17), 30 g of carbohydrate that escapes absorption in a day could produce more than 10,000 mL (ten liters) of hydrogen gas. That is a huge amount of gas!
When stomach acid is sufficient and carbohydrates are consumed in moderation, they are properly broken down into glucose and rapidly absorbed in the small intestine before they can be fermented by microbes. However, if stomach acid is insufficient and/or carbohydrates are consumed in excess, some of the carbs will escape absorption and become available for intestinal microbes to ferment.
Other Supporting Evidence
Dr. Robillard also argues that if gas produced by microbial fermentation of carbohydrates causes acid reflux, we might expect that reflux could be treated by either:
- Reducing bacterial overgrowth, or
- Reducing carbohydrate intake.
He points to two studies which demonstrate this. In a study by Pehl, administration of erythromycin (an antibiotic) significantly decreased esophageal reflux. (6)
In another study by Pennathur, erythromycin strengthened the defective lower esophageal sphincter in patients with acid reflux. (7) To my knowledge, there have only been two small trials performed to test the effects of carbohydrate restriction on GERD. Both had positive results. A small case series showed a significant, almost immediate resolution of GERD symptoms in obese individuals initiating a very-low-carb diet. (8) A more recent study found that a very low-carb diet decreased distal esophagus acid exposure and improved the symptoms of GERD. (9) Perhaps most importantly, the magnitude of the improvement was similar to what has been reported with treatment with proton-pump inhibitors (acid suppressing drugs).
Some researchers now believe that Irritable Bowel Syndrome (IBS) is caused by small intestinal bacterial overgrowth (SIBO). (10) A study performed at the GI Motility Center in Los Angeles in 2002 found that 71 percent of GERD patients tested positive for IBS—double the percentage seen in non-GERD patients being examined. (11) The high prevalence of IBS in GERD patients combined with the recognition that bacterial overgrowth causes IBS is yet another line of evidence suggesting that bacterial overgrowth is also a causative factor in GERD.
Final Comments
To summarize, low stomach acid contributes to bacterial overgrowth in the bowel which in turn can lead to carbohydrate malabsorption (due to decreased pancreatic enzyme secretion). Malabsorption of carbohydrates, as Dr. Robillard has pointed out, increases intra-abdominal pressure and causes GERD.
Where Dr. Robillard and I differ is that I believe low stomach acid is the primary problem with GERD, with carbohydrate malabsorption playing a secondary role. I do think that improper digestion of proteins can, in fact, lead to GERD, whereas Dr. Robillard states in his book that putrefaction of proteins is more likely to cause flatulence. This may be so in most cases, but I’ve seen several patients in my practice on very-low-carbohydrate diets who still experience heartburn, which improves upon restoring proper stomach acid secretion (which we covered in another article in this series). In the Part III of the series I discuss the connection between GERD and H. pylori, and further evidence supporting the theory that GERD is caused by bacterial overgrowth. Read on!
Better supplementation. Fewer supplements.
Close the nutrient gap to feel and perform your best.
A daily stack of supplements designed to meet your most critical needs.



While my symptoms are similar to those above they are slightly different so hoping someone can give me advise. For about 6+ years I’ve had the following symptoms: in the afternoon (typically after lunch) I get a burpy feeling where I feel air coming up but it get trapped so I cannot belch. I also get heartburn typically at the same time. The only way to alleviate the symptoms is to dry heave. I don’t throw up any food or stomach acid but the action of dry heaving is the only thing that helps. I’ve been taking Prilosec for 6+ years (?) now and recently my symptoms have gotten worse. Is the Prilosec making things worse? Is my heartburn and burpy feeling related? What is my burpy feeling? Any help is appreciated. I’m scared to eat as I’m not sure what is causing my symptoms.
Where does hiatal hernia fit in to this discussion? I have had decades of heartburn (since my 30’s), and an endoscopy in January of this year found hiatal hernia, Barrett’s Esophogus, and lots of surface ulcers. 20 mg Omeprezole was a miracle cure for five months, but then began destroying my intestinal system. Got off it and then had terrible rebound symptoms (including lots of mucous in the back of my throat causing a constant cough). Anyway now back to Zantac once (occasionally twice) a day. Want to get off meds. Any advice?
Constant cough. I had it for six months. Doctor put me on medication that dried up mucus membranes. It worked but had bad side effects. Stopped medication and cough came back. This is what I found out. I have an hiatus hernia. If I lay flat in bed acid can migrate into the osophagus. The pepsin in the acid gets embedded in the osophagus. This causes inflammation and irritation when fluid passes and activates it. During normal bodily function we pass mucus from the back of the nose down the throat around a litre a day. Rough guess. This causes irritation and makes you cough. Cure. Put a teaspoon full of bicarbonate of soda in 280ml of water and drink it while you watch tv. Alkaline water neutralises the pepsin in your throat instantly. This cured my cough. Digestive enzymes with betaine hcl cured my bloating and chronic gas(belching). If I drank water it gave me gas I added lemon juice to the water and it makes it more like stomach acid. This made a big improvement in my health. Only used the lemon juice for about month. Then I started experiencing reflux something new for me. This I realised was being caused by my home made fresh bread. I baught an adjustable bed so I don’t sleep flat. I’m the best I’ve been in years. One other problem I had which confused things was two or three times a day I would turn really queer and ill and this forced me to lay down. I thought it was the Vagas nerve being trapped. I made the connection with coffee consumption. I stopped all caffeine drinks and bingo I now feel cured. Ant-acids made me worse. Hope this info helps.
I have doubts about the mechanism described in this article, which I understand to be this: Bloating in the stomach pushes acid up through the sphincter to the sensitive esophagus. I’ve begun having heartburn regularly, but zero stomach bloating and normal gas compared to before. I do know that if I increase my vegetables (working on that!) then the heartburn subsides. When I eat acid-forming foods (Google it) heartburn increases but alkaline-forming foods cause it to decrease. And, if I take antacids the pain does go away. This is consistent. Also, I’ve been taking Solaray High Potency HCL with Pepsin 650mg for a few weeks, to no effect. Frequently twice a day. I know a pill isn’t going to solve my problems; I know I just need to get in there and eat my danged broccoli.
All of this suggests to me that I do indeed have too much stomach acid, as the conventional wisdom goes. Thoughts?
Making milk kefir solved my digestive issues. Acid reflux, bloating……. Homemade kefir has more and superior probiotics than commercially produced probiotics or commercially produced kefir. It is a live food. Of course you still need veggies but the microbiome is a largely ignored subject by most mainstream medical docs!
Do u have the recipe for homemade Kefir.
Hello,
I’ve been on Prilosec for about three years. It worked well, and was cheap, but I wanted off.
I stopped taking it about three weeks ago. The first two weeks were an on-and-off hell. But with a simplified diet, and sufficient fluid intake, I’ve been symptom-free for about a week AND FEEL TERRIFIC. Seriously, I can’t remember feeling this good for years. In my case, I’ve found that fried foods and red wine are completely off limits. I’m slowly adding foods to my diet without consequence. Yesterday, I had a grilled pork chop without any repercussion. There are foods that I suspect are also off limits, based on earlier experiences. These would include; nuts, cheese, and tomato-based products.
Milk kefir…..homemade is best, full of probiotics!!
I have been on 20 mg of prilosec for 4 years. I want to wean myself off. so, my doctor said to go cold turkey but my pharmacist said to skip the pill every other day for about 2 weeks and then every 2 days and so forth. I skipped it twice and I feel air burping throughout the day today. I feel slight acidic. 🙁 Is my body just going crazy with not knowing what to do? Will this pass? Should I just keep the weening? What should I take in the meantime to just keep it under control instead of a PPI? Also, when I started the Prilosec I also got IBS and yes I did have bacterial overgrowth and had to take an antibiotic to get rid of that. The doctor said that will keep happening. Did I read the article correctly when it said to stop eating carbs? Eating acid really isn’t the problem but eating foods that relax the sphincter muscle is. So. How do I get my sphincter muscle to work properly again. My doctor said the only way is through surgery and he doesn’t recommend that. Please help. How do I do this? What should I eat? Thanks SO much.
I’m going through something similar at the moment and I’m devoting a large portion of my time to figuring out how to handle this complex situation.
I strongly recommend reading “Why stomac acid is good for you”. Apart from that there also is a non-surgically way you can enhance your LES muscle:
Research has shown that breading exercises train your diaphragm muscle which will help you to keep more pressure on your LES. This takes several weeks of discipline but it alleviates up to 50% of the symptoms.
Stress is of course counter-productive since you will not be using a proper breathing technique.
Good luck and stay strong!
Does anyone know how to handle acid coming out your nose and I have been told I don’t have hpylori through a camera down my throad and a snip, and now through other testing I have been told I do ..so i am treating it with Mastica. Anyone have any tips as the hot air coming out my nose is driving me crazy!
I’ve been trying orange peel (n-limonene) which I pretty much have to order online or directly eat the orange peels. I’ve been taking 250 milligrams which is 25 percent of what is recommended. In two months, I’ve haved the acid reflux medicine, don’t feel bad in the morning and am starting to go for the end goal post which is no acid reflux medicine.
Which test came back positive for h pylori?
I have been on PPI’s for 10 years. What is the safest way to wean myself? I have been diagnosed with SIBO, gastroparesis, IBS, Hiatal Hernia, gastritis and esophogitis and chronic constipation.
The PPI’s are causing ALL those symptoms. Get off, Now it will shock your body and acid will ramp WAY up and you will be miserable for a week or so but just use antacid tablets to get thru it, do NOT go back on PPI’s. PPI’s are extremely dangerous and make drug companies BILLIONS$$$$
PPI does not cause the esophagitis and gastritis. I had these BEFORE being on PPIs. Reflux was the reason I needed to get on them. Symptoms have improved but are not gone.
I would suggest considering a fecal transplant.
Addressing (testing initially) through a stool test like GI Effects Comp stool analysis.
Faecal transplant by an approved/recommended clinic may be most effective in the shortest amount of time.
Get a UREA breath test to determine intestinal colonization of bacteria (SIBO). Treatment regimen is Rifaximin 1200 mg daily for 10 days (divided into 400 mg doses 3xs daily). HCI with Pepsin for 3 weeks post treatment.
I was diagnosed with GERD at 39 after 20 years of powerful belching and 2 years of periodic vomiting after eating more than small amounts of food at a time. An endoscopy showed an inflamed esophagus and I was put on high doses of prilosec for 2 weeks. After a week and a half I developed a 2 week intestinal infection that was only ended they antibiotics. I am currently taking hydrochloric acid pills when I ingest protein and limiting carbs and sugar. I never had heartburn as a symptom but the belching and vomiting seems under control. So, I am curious. Do you think it is possible that growing up for the first 15 years of my life as a vegetarian (fish only) could have trained my body not to produce as much stomach acid? May be a long shot but the appearing need for “acid” when I ingest protein makes me wonder.
Karen,
I was was similar situation. Had acid reflux for 10 years. Bad bacteria could be causing the problem. They need to be replaced with good bacteria. So to do this , you introduced good bacteria by pro-biotics. I took pro-biotic IFlora, it cured my acid reflux in three days. On the same weedend, I did not have acid reflux. Pro-biotic are highly strain specific, so I did not find other pro-biotic effective,. Look for my comments on the amazon. You can also try Kimchee, it should have similar affect. You can try white Kimchee which is bland in taste. Kimchee is highly affective , about 99% of bacteria attaches to the digestive tract. Wish you all the best.
Hi, I was suffering from Eating Disorder (Bulimia Nervosa) for 15 years. I also suffered from Gastritis since teenage. I finally manage to stop ED. But after many years I realize that it had done more damage to my GI tract. My gastritis got worse, valve damaged, GERD grade 2 (almost 3), IBS, bloatness, weight gain, etc. Doctor also adviced me not to do any exercice that could put pressure on the tummy and valve. I tried Digestive Enzyme and it helps a little. Other than that, I also noted that i’m unable to take anything made of oats, soya, wheat and few other grains. They cause severe heartburn and I also a sensation as though there is a lump blocking at the end of my esophagus whenever I try to swallow something. I tried a Probiotic supplement yesterday but it too causes severe heartburn, or could it be the steamed bread I ate? It is so frustrating to feel unwell all the time.
Bread does it to me almost every time, oats, barley, sugar, alcohol unless if been on a very clean diet, protein, veggies, fruit…only grain/starch , rice or potato
Hi Chris,
I really want to try what you are suggesting but concerned that by taking HCL it’s going to aggravate my gastritis further. Do I need to try to reduce the inflammation first before I try to supplement with HCL?!
stay away from ppi pills. i had only minor gastrits. after started to use ppi and then reflux happened. Modern medicinal treatment sucks ! after reading articles on thousand pages of diggestive system. i found out solution on herbal remedies… apart from low stomach asidicity . Heartburn caused by SIBO. Small intestine Bacterial Overgrowth. ! That’s what PPI pills make ! They shut off acid mechanism of stomach and let viruses bacterias fungus go and settle in small intestine. First of all. When you are in remission . Clean out those parasites from small intestine. Small amount of Mastic gum, 1 Clove bud, 1 teaspoon Cinnamon, Ginger, Pine honey combination works well for me. Anyways Solution is in your hands. ONly you can find what cures you… !
totally wrong. cinnamon and ginger will irritate the hell out of your stomach and cause a burning sensation to the already sensitive area. my reflux happened BEFORE taking PPIs.
What a tricky disease to deal with and unfortunately, we all have to eat! My primary symptoms are with chronic heartburn. Although I’ve had remarkable results taking HCL with pepsin, sometimes it’s difficult to get the dose right.
In 1981 I had my gallbladder removed. I see a number of comments from people with the same course of treatment having a lot of issues with their stomach “dumping”. That happened for me, too, but as the years have passed, I no longer have that problem. But that got me thinking about how my organs likely have been moved around, maybe some scar tissue formed, and could be impeding good digestion and started reading about visceral manipulation (among every other treatment you can read about on the internet)
Recently, I had a treatment by an osteopath. I went in cautious but optimistic. Even after only one treatment, I have noticed a difference. Particularly at night whereas I can now often times lay on my right side.
The osteo’s recommendation was that if he didn’t get significant results after three treatments, then he would recommend another course of treatment (meaning something other than osteo).
It made sense to me that maybe my organs weren’t getting the room they needed to function optimally what with sitting at a computer all day!
My recommendation would be to give an osteopathic treatment a try.
Sandy
Hey
I’m not sure who’ll get to read this or will respond, but I’m really, really seeking some advice. In my many, many searches I’ve come across your (chris’) pages constantly, and while they offer some great information…I’m still stumped on what to do.
Basically for the past 3 and a half years I’ve been having continual digestive issues, seen a gastro doc and in doing so…my problems have only gotten drastically worse to the point of where I’m terrified to eat, either because I’m feeling sick or I’m scared of what might happen if I do eat certain foods. I was put on PPI’s, and a year of use gave me sibo…antibiotic courses didn’t help, or if they did I was lucky to get a day of relief after a week of misery of added symptoms from the medicine.
Anyways, my symptoms now are as follows, constant (and I mean, CONSTANT, never ceasing) stomach pain in right quadrant, bloating, cramping, queasiness…three-five bathroom trips in the morning, with either gas/pain before or following the last two, this has been steady for a year now.
Things I’ve tried, probiotics, digestive enzymes, ACV, I did try betaine HCI with pepzin…but eventually this aggravated my stomach, I may have been taking too much and given myself gastritis, as now I’m having a lot of burning/cramping on the left side of my stomach too.
I’m meaning to see a naturopath…but can’t afford it right now, I’m in such misery everyday, not to be dramatic it just never seems like it will end. I limit my carbs, try to have vegetables, am wary of fruit as it can feed the sibo, drink plenty of water (always have to pee…not very happy about that) I have tried various antimicrobials, (GSE, oile of oregano, olive leaf extract, goldenseal…) but found these to be too harsh at times for me, and they never helped with my stomach issues obviously because they don’t do anything for digestion other than get rid of access bacteria, but not enough.
I can’t tolerate vitamin c…like, at all, I tried this under someones advice and it made me have horrible pains before having to go multiple times. I used to love organes, organe juice, but within minutes of eating them I have to go to the bathroom.
…I foolishly had my gallbladder removed under doctors recommendation nearly two years ago, and things have only gotten worse since that event too. I’ve done everything I was told and I’m more messed up than ever, I fear I’ve done irreversible damage. So off and on I have to deal with Bile salt d…when I’m not constipated and barely passing anything because I can’t evacuate my bowels properly.
I’m just so distraught, I know stress doesn’t help, I try hard to relax, but I’ve not been able to lie down on my back and REALLY be comfortable because of gas and pain in years…I can’t even remember what that feels like. If Chris, or someone else can suggest something I can try…or something I can do, I know I need betain but my stomach is really raw right now, and most digestive enzymes contain this, or protease which I read can also aggravate the stomach lining so I steer clear of those too.
Ken, I would say that I have experienced about 75% of what you have written here. Growing up I had mild issues, so my parents didn’t allow me to eat a lot of junk food. As I have gotten older, my problems gotten progressively worse. The last 7 years had been the worst. I’ve seen 13 doctors in last 7 years. Regular doctors, gastro doctors, allergists, etc. I got to where I would just drop the doctor if they wouldn’t listen to me or pushed another drug. I was diagnosed with GERD when I could no longer sleep laying down without regurgitating acid and bile. I was given Prilosec and Nexium, which made my problems even worse. I finally saw a nutritionist and naturopath because I knew it had to be something I was eating. I couldn’t sleep, my hair was falling out, I had painful digestive issues, my skin turned dull and started getting itchy rashes. I went through an elimination diet to test major allergens. I could go on and on, but in a nutshell, I was diagnosed this past June with Celiac disease. I have been on a very strict gluten free diet and I already feel like a million bucks. My thyroid readings were all normal except the TPO Antibodies and I am currently being monitored for Hashimotos. Since being gluten free, the antibodies have dropped considerably and my hair stopped falling out.
If I were you, if you cannot afford a gluten allergy test (anti-gliadan antibodies test) you should do a strict elimination diet. So many things contain gluten, so you have to read every label. Gluten is in wheat, barley and rye. IF the label does not say gluten free, don’t eat it. Test this for 4 weeks. Be strict. Eat clean. Basically just lean meats, vegetables, and potatoes and rice in moderation. It doesn’t hurt to try. Your story is very similar to mine. My own father had worse problems than me. Celiac is genetic. Good luck.
Hey
Thank you for responding to me, I really appreciated it.
I was tested for Celiac I think, came back negative, but it might be something to look into again. I (briefly) cut out grains, it was hard given my lifestyle but do recall some improvement, nothing miraculous but enough to be noticeable.
I’m not sure if it helped with the ritual 3-5 bowel movements in the morning though, that’s the most frustrating thing for me right now. I’ve inquired to countless forums and tried countless suggestions, and nothing really seems to fix that, and it’s not something I want to have to deal with anymore, having to put everything on hold until 3-5 pm when I’m finally done going #2, it’s stupid. But I’ll just have to try gluten free for longer perhaps, it cuts out 85% of what I seem to end up eating.
just because you tested negative for celiac doesn’t mean that you are not sensitive to gluten or that gluten isn’t causing you issues…
do an elimination…for 30+ days. it is well worth the test.
Hi Ken, you may want to look in to whether or not you have a form of chronic pancreatitis. It is a very under diagnosed condition, and it can cause many many issues with digestion, nutrient and fat absorption as well as chronic morning diarrhea. A person does not have to be an alcoholic to have CP. Pancreatic enzymes (high dose RX not OTC) are really the only thing that can help.
Even if you don’t have Celiacs, get tested for grass allergies. I’ve always known I was allergic to grass and felt like an idiot when my doctor said “oh so you don’t eat wheat and grains”….because those are essentially grasses. I stopped eating grass and stopped taking stomach meds. I also didn’t know if you have pollen allergies to trees you have to cook foods like carrots due to cross pollination. I had my son tested for pollen and my doctor said nothing. I heard it from a friend with the same allergy who solved my mystery for me.
I was tested for Celiac and negative. BUT when I eat gluten free blue corn chips, I get horrible reflux. Hmm..
I tested negative for celiac but after going to an allergy specialist her mentionef that corn, oats and wheat are irritants to my stomach pain
Corn is hard to digest and could be a sign of intolerance of you do not feel well after…same pain happens to me which makes sense based on his testing.
Ken – I have these same symptoms – almost exactly. Every time I eat, and sometimes only after having water, I will start to bloat, pain up under the right rib. When the bloating is really bad, the pressure feels as though there is a tire up under the ribs – I feel it front and back and on both sides.
I have to be cognizant of the timing of my meetings to determine when I can eat in the morning because once I eat, the bloating starts and the trips to the bathroom soon follow. I alternate constipation and soft stool/D with bile.
I was diagnosed with bile reflux via endoscopy but I have to believe that there is more to it. I feel like the bile reflux is a symptom of something else and have been investigating SIBO. It is so frustrating.
These symptoms have plagued me on and off since my GB removal in 2007.
Honestly sounds like a gallbladder issue. I lost weight too fast and then struggled to hold down water. Was puking bile due to (what i’m guessing) something getting stuck in a bile duct. I’m so sorry you’re going through this. I almost stabbed myself trying to relieve the pain.
Have a look at Dr Sarah Myhill’s detailed website all about gut problems & their solutions. Very helpful for many people https://www.drmyhill.co.uk/wiki/Category:Bowel_Problems
Good luck, Chris
Hey, why not try panchkarma? Its Indian method of cleaning the body. You will need to stay in Ayurveda Asharam for 15 days. We always prefer herbal ayurvedic medicines instead of Allopathy. There are asharams in Germany and Switzerland also. You can research first and then decide.
Tonya,
In case you still may need or want to try again I could not tolerate vitamin C in the asorbic (can not spell that) acid form actually caused bleeding so I avoided all Vitamin C until I found Synergy’s which is made very different than what you usually find on the market. I now can use high doses if I want with no issue: https://www.thesynergycompany.com/ProductDetails.asp?ProductCode=1PCPO
I could not tolerate and B complex vits. either however I can now do two a day using the synergy products.
WHAT SYNERGYS HOW DOES IT WORK WITH ACID REFLEX THANK YOU
Hi Ken,
It sounds like your liver is highly congested and is having trouble producing enough bile to emulsify fats and proper digestion of the foods you are taking in. The problem was compounded by having the gallbladder removed so it makes sense your symptoms seemed to have gotten worse since the surgery. I highly recommend reading up on the Hulda Clark Liver Flush. It has remarkable benefits. If you go to an online health forum called CureZone and type in liver flush under the search, you will read stories upon stories about how it has changed people’s lives. I am one of them. You may need to read up on whether or not the flush is modified for someone with no gallbladder. But I don’t think it’s an issue. There is a health guru named Andreas Moritz who also goes into great detail about why these liver gallbladder flushes are so vital to our our health, for the sick or poor.
I wish you the best of luck.
Hi Ken,
you shld try gluten free diet. maybe u have IBS or COLITIS but most important is what you eat. stop all the herbal meds first. you have to fix the damage.
Have you tried sauerkraut ? Its very good for digestive issues and cost effective too ?
Try incorporating natural yoghurt if you can, it is soothing for the stomach.
Best wishes
sauerkraut? that would aggravate symptoms for a lot of people.
Low pH is needed to properly digest food and kill bacteria, etc, Kresser and others never mention that pH is raised when there is more liquids to dilute the acid. I need water, but I drink a lot about 30 to 60 minutes before my meal, then I drink no liquids with my meal, I theorize that water passes through the stomach quickly without stimulating much activity. My stomach pH presumably is very low and it digests whatever is in it well. I also don’t eat much carbohydrates to begin with,
Diet of brothy soups, until inflamed gut is healed. Might take 6-18 months.
Have you been checked for H.Pylori? Ask your doctor for a blood test or breath test or stool test.
Also, try to get an endoscopy and colonoscopy to maybe see what’s going on. Sounds like you might have some gut inflammation. Eat a vegan lifestyle and see if that helps. So sorry your going through all this. I too have had stomach problems the last 4 years off and on. Your story sounds like mine.
Get well soon!!!
Hi Ken,
I hope your gastro has recommended cholestyramine for the bile salts D. I have IBS with GERD issues. I used to have ‘episodes’ every 2-3months, then had my gallbladder foolishly removed as well. It made my D and GERD episodes into a daily struggle, often having ‘dumping’ issues every morning and unable to tolerate certain foods. Though I still have issues and flare ups, I am able to keep the daily D at bay with 1 scoop per day of cholestyramine. And I’m off my PPIs, which did nothing for my GERD and helped acquire Cdiff. Do not take PPIs!! I find daily D relief and esophageal soothing from cholestyramine. Be careful, as too much can cause constipation and bloating with increased GERD symptoms. I was first prescribed 2scoops per day and found decreasing to 1 was the best fit for me. It tastes gross, but saved me and allowed me to be able to leave my home and get out and live again!
I have acid and bile reflux and have noted that Gaviscon helps greatly with reflux. Give that a shot if you’d like.
I can attest to these articles completely. Let me know if this sounds familiar to anyone. I went in for Gastritis about 6 months ago. I was prescribed Nexium and was told to take religiously for 4 months. Nexium provided absolutely no relief after months of taking, Dr. recommended to up the dose and keep taking. Eventually I developed more symptoms rather than less, extreme bloating, Intense pressure/pain around the sternum, excessive gas, heartburn, ucler-like pain, and when I would eat food it would literally sit in my stomach for hours. Friends and family began to think I was a hypochondriac with all the symptoms and issues I was complaining about. Dropped my primary care physician out of sheer frustration and got a new one. To my surprise she said the exact same thing, ‘too much stomach acid’ and prescribed me Protonix. Better results, but I kept noticing that most of the symptoms would linger while some went away. Finally I did some research of my own and came across ‘not enough stomach acid’. This was like coming across the ‘Holy Grail’ for my GERD. I purchased Gastrazyme, Manuka Honey, Licorice DGL and most importantly HCL w/ Pepsin. Gastrazyme is known to heal stomach lining and is a very efficient way to get that Vitamin U supplement people with GERD need. The Manuka Honey is known to have extreme healing properties. Licorice I took to for the immediate pain with some success. I will say everything seemed to keep my symptoms at bay, but did not clear 100%. Then I started taking HCL w/pepsin. I too was skeptical about taking a magical pill after being lied to and led astray by my Dr.’s. I can attest that the first day I took HCL w/pepsin I felt an immediate relief in Pressure, burning, gas. I am a week into taking this and my symptoms have alleviated 75% (and rising). I have been in extreme discomfort so long I almost refuse to believe its working. I also should recommend what every other comments says as well, cut down your carbs completely. Find your trigger foods and also cut them out. For me its coffee, alcohol, some spicy food, and nearly all carbs. Feel free to ask me any questions or advice if you need it. Please keep in mind that all remedies work different for each person, please do your own research before you spend $100+ on a cure. Good luck all, I know dealing with this takes you on the brink of insanity..but there is hope.
I would also recommend to anyone suffering from GERD symptoms to do a parasite cleanse and follow it up with high doses of probiotics. My symptoms started to improve dramatically after I did the parasite cleanse and continue to do so. I did the herbal one, but you can also do it homoeopathically. The other thing that has made a difference for me is to heal my stomach with high doses of amino acid – like l-glutamine. For me, the results last longer when I use ISO whey powder in my smoothies. Less burping, and when I do, it’s because I’ve eaten something that I can’t digest, but that usually goes away with a couple of 650 mg HCL with pepsin.
Good luck!!
Where do I find HCL w/Pepsin? Please email me at [email protected] I noticed the pressure and indigestion after eating bread, greasy foods, tea and coffee. Now I am waking up in middle of night with it I only have baking soda and water at this point and its not working now that this is progressing. thanks
Were you diagnosed with a hiatal hernia?
Hello,
One very honest opinion from my side. I tried homeopathic treatment for GERD with a medicine known as NUX VOMICA.
Trust me, it worked very well. It has been more than 4 months that I have fully recovered from GERD but sometimes when I feel high acidity I take Nux Vomica capsules.
Importantly since it is not an allopathy medicine, it has little side effect on body.
You can consult a homeopathic doctor regarding this.
God bless you all.
Thanks,
Suhel
I do not have pain in my stomach or anywhere else. I just have acid in my throat. I had a little pain under my right shoulder blade but that has gone away. It is mainly the acid in my throat which has been there for about a month with little relief. Does anyone else have this? Prilosec has offered little to no relief.
Josh,
I am relieved to read your article. I have been an emotional wreck since all my diagnoses of IBS, GERD, Gastroparesis, Lactose in Intolerant and most recently, Severe Intestinal Bacterial Overgrowth (SIBO). The only symptoms I’ve had my entire life (I’m 33) was painful bloating, excessive gas, pressure and constipation. Everything went undiagnosed until this year. I was always pushed pills as a young woman. In July I received the IBS and Lactose diagnoses (mind you I’ve always had a really bad diet). Then I got diagnosed with mild gastritis and esophagitis. The Dr. prescribed me Omeprazole for that which I dutifully took. After two months of taking that, I started new symptoms I’ve never experienced before: feeling full really quickly and last all day long. I went in for an already scheduled Gastric Emptying test, which came back with slow gastric emptying. When I got this diagnosis I was so confused. I didn’t understand what was happening as I never had those symptoms before. I always have been able to eat normally. Of course the Dr. ups my dose of Omeprazole and puts me on Linzess (which was a mystery to me since my constipation had been taken care of…I’ve since stopped the Linzess). Since the start of the Omeprazole, I had been able to go back to normal eating. I was doing wonderful on a low FODMAP diet. Then I got lazy and began to eat all the bad foods again and had a flare up with the acid reflux for the last 2 weeks. I called my dr. who switched me to 80 mg daily of Nexium. I was really unhappy with this is I would rather not take PPI’s so I’ve only been taking 40mg daily, but I switched to a liquid soft diet. I found some relief with this, however, I still feel the huge lump in my throat. Now fast forward to my latest diagnoses of SIBO. I was excited to get this diagnosis because I believe this has been my problem all along. When I asked my Dr. if this was causing my acid and my Gastroparesis, she told me no. This made me really angry as the literature suggests otherwise.
Now, I am just frustrated and fed up.
However, the point I was trying to get it, is that I am relieved to read that you switched to a more natural way to eliminate your symptoms and hopefully clear what’s ailing you. I to have been contemplating switching to a more natural medicine. However, I am apprehensive as I don’t know if I will have bad withdrawals from the PPI’s. I’ve only been on them since late August, so I am guessing it wont be that bad. I too, read to take the same items that you have been taking accept the honey. I am interested in hearing further how your treatment is going.
You are giving me hope!!
My Pulmonary doctor said the same thing. He believes that due to the Gerd, I am getting chronic sinusitis and lung infections. He put me on that Erythamacin antibiotic to help my stomach. He is calling my gastroenterologist to discuss what needs to happen for my IBS, gerd, hiatal hernia, fall bladder problems, constant low grade fevers and constant pain in my belly, chest, throat. The vomit is projectile, it spews out when I can finally burp. He is scheduling a surgery or whatever to check each of my lungs. He belies my asthma and COPD are due to chronic infections due to the stomach fluid in my ears, nose, and aspirated into my lungs. Pray he got it right!
I ‘ve had no gallbladder since I was 16 and am now 60. I’ve had all the symptoms of gerd, but mostly started when I’d have to burp only by sitting up or getting up. Dr. told me to quit smoking and drinking coffee. so far I’ve cut back on coffee and it’s tougher to give up cigarettes,but, when I have flare ups I notice cold water can hurt going down, and sometimes it’s hard to think of eating. Have lots of sinus issues. Papaya enzymes help with eating. I do probiotics and aloe vera juice. Anyone else tried these things? Also am hypothyroid and believe that has something to do with all of this, but of course, Drs will not listen and only keep you in there desired amounts of synthroid.
hi
I am ready to die. I have so much pressure and hot air coming out my nose and mouth. I don’t even know where to start.
Please don’t say that. I feel your pain everyday. My stomach will just blow up like a soccer ball at anytime. Everything I eat. Everything. Gives me heartburn..
I am so sorry for all of your suffering! Every professional seems to have a different opinion, and the sad thing is that they may all be right in some regard.
For years, my indigestion and reflux were completely relieved by HCl with pepsin and DGL (when I felt any kind of discomfort). Then for unknown reasons it stopped working about a year ago. I wonder if it may be related to thyroid treatment, which I stopped just to see if that was the cause, but the intestinal problems continued, so I went back on them.
Does anyone know if there is a relation between thyroid meds and GERD and reflux? And why would the HCl stop working?
When you say burning, did your stomach itself burn too? I have had horrible GERD for 14 years and I am in 30 so I was young when it started. I know people say lose weight and all that but when I was diagnosed I was 16 5 8″ and 160 pounds I also ate healthy and jogged and lifted light wieght 6 days a week. Now my weight have fluctuated and I feel like crap all the time. I have Nexuum but I am getting extremely concerned about the long term side affects. I don’t k is why to do anymore and honestly I am beginning to hate eating. Even water feels like I a
Pouring acid into my stomach sometimes. I do have other health problems. However, I feel so lost with conventional docs because all they do is throw pills at me. I am sick of feeling this way!! Any suggestions ?? I have tried the “stops acid reflux” it has apple cider vinegar, garlic and ginger; it helps sometimes but not always and I am also extremely sluggish and no matter what I do I keep gaining weight almost weekly. Frustrated! Any suggest uti s from anyone would be wonderful
Hey Shaunna. Have you ever had a colonoscopy or endoscopy? I would also ask for a H. Pylori test from your doc. I hate conventional medicine too! See a holistic doc if you can.
Feel better!!!
Josh, Can you tell me more about GastraZyme? How do you take it?
I had GERD and I was on pantoprazol for 5 months. Then my pantoprazol medication ran out and I got GERD again. I did not buy medication again though.
For completely different reason, I decided to go on very low-carb diet, Surprisingly my GERD vanished after a week being on low-carb diet. I only ate chicken and red meat and vegetables with lots of spices. Then after three month and loosing 3 kg I started to eat carbohydrate. After a week my GERD started again!
Interestingly, whenever I eat 3 consecutive meals containing rice or potatos, I get GERD.
Anyway, I’ve started low-carb diet again and don’t have GERD since. I hope more research will be done about relation between low-carb diet and GERD.
i have Gerd it has been 2 days , i am on medication now for 30 days. trying to make sense of all this… has anybody experienced EAR pains ? more often left ear pain. i am deeply concern, i don’t want to over analyse, however reading reviews, for most people ear pain was not there!! Ear pain usually takes the situation to a whole new level of throat cancer!
Heartburns, no vomiting, throat pain continuous, ear pain very often
Help people what is this ?? 🙁
I’ve had a 22 year history of post nasal drip ( probably due to gerd or allergy or something unknown) and sometimes during a sinus flare up i get ear pain or pressure due to blocked middle ear ( and a nagging 2 week headache). I got things checked out only a couple of years ago and got put on pantoprazol for 6months and still got the occasionally ear pressure or pain. So, the GI put me on some amitryptiline ( low doses work on nerve pain) and that seemed to work. I haven’t taken PPIs for almost a year and quit amitriptiline a couple of months ago. But this last week I’ve had ear pain ( right ear), headache and tight throat again but it usually goes away.
I think you’ve got to have some serious cough, swallowing problems and hoarsness before you start thinking about cancer. Other things can cause ear pain.
But it’s probably a good idea to have regular visits to an Ear Nose and Throat specialist and a GI to see if there’s any serious long term irritation in the eosophagus and airways. I had 2 visits to both GI and ENT in the last year and everything so far seems fine.
Sharbel
I had inner ear pain for 3 months. I searched for ear pain without infection and found many articles which referenced GERD.
Have you considered tonsil/adenoidal issue? I had a lot of earaches with seemingly no cause and I found out it can be from having enlarged adenoids
Yes! Every other doctor ignored me when I stated I wake up with bad stabbing ear pains and that they fill up with fluid. The Pulmonary doctor, just listened and his eyes glistened and he said I think I know what is wrong with you. He has scheduled two tests, called my gastroenterologist and if he doesn’t agree, he is referring me to another one who practices at another hospital in my city. Then, he put me on antibiotics. I finally have hope!
I have noticed my ear pain related to eating dairy. This has only been the last few months. I had a bad cold and the ear pain never went away. The docs checked it and said there is fluid but no redness. That’s when I noticed it correlated with dairy. Since then, I have discovered I also likely have Silent Reflux.
Is the pain conatant ?
Have to find a way to deal with gerd.
Just started a low carb diet today. For the past few months I’ve been taking up to 8 tums a night for my heartburn b
Apologies. Phone sputter. As I was saying, for the first time in months I have zero heartburn. I completely agree with this article. Some combination of acid levels and or carb intake has been killing me. Can’t say this is the cure as of yet but for the first night in a very long while, I’m completely heartburn free. Thanks for the article.
I like your theory regarding carbohydrate and gerd.
I get gerd reliably from any of these things:
– alcohol
– chilli
– coffee
– bread
Drinking a milk chaser after the chilli and coffee helps with those but not the others.
If I abstain from all of the above for 2 days my gerd goes away completely. It’s a shame though: I like them all!