This is the second article in a series on heartburn and GERD. If you haven’t read the first one, I’d suggest doing that first.
The idea that heartburn is caused by too much stomach acid is still popular in the media and the public. But as Daniel pointed out in the comments section of the last post, anyone familiar with the scientific literature could tell you that heartburn and GERD are not considered to be diseases of excess stomach acid.
Instead, the prevailing scientific theory is that GERD is caused by a dysfunction of the muscular valve (sphincter) that separates the lower end of the esophagus and the stomach. This is known as the lower esophageal valve, or LES. The LES normally opens wide to permit swallowed food and liquids to pass easily into the stomach. Except for belching, this is the only time the LES should open.
Here’s the key point. It doesn’t matter how much acid there is in the stomach. Even a small amount can cause serious damage. Unlike the stomach, the lining of the esophagus has no protection against acid.
Free eBook
Learn More about Heartburn and GERD
Download this free eBook to discover the little-known causes of heartburn and GERD, and find out how to get rid of the problem forever.
"*" indicates required fields
I hate spam, too. Your email is safe with me. By signing up, you agree to our privacy policy.
We’ve Been Asking the Wrong Question
In an editorial published in the journal Gastroenterology, the author remarked: (1)
Treating gastroesophageal reflux disease with profound acid inhibition will never be ideal because acid secretion is not the primary underlying defect.
I couldn’t agree more. For decades the medical establishment has been directing its attention at how to reduce stomach acid secretion in people suffering from heartburn and GERD, even though it’s well-known that these conditions are not caused by excess stomach acid. Instead, the question researchers should have been asking is, “what is causing the LES to malfunction?” Since it is universally agreed upon that this is the underlying mechanism producing the symptoms of GERD, wouldn’t it make sense to focus our efforts here? That’s exactly what we’re going to do in this article.
GERD Is Caused by Increased Intra-Abdominal Pressure
It is well accepted in the literature that GERD is caused by an increase in intra-abdominal pressure (IAP).
For example, several studies have indicated an association between obesity and GERD, and one paper in Gastroenterology concluded that increased intra-abdominal pressure was the causative mechanism. (2, 3) But while I agree that all of the currently accepted factors play a role, I do not think they are the primary causes of the increased IAP seen in GERD.
The Two Primary Causes of Increased Intra-Abdominal Pressure
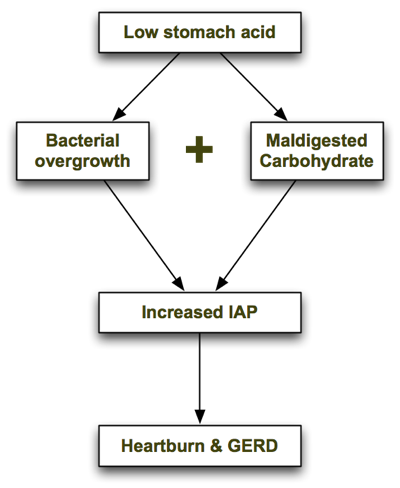
In his excellent book, Heartburn Cured, microbiologist Dr. Norm Robillard argues that carbohydrate malabsorption leads to bacterial overgrowth, resulting in IAP which drives reflux. Dr. Robillard makes a strong case that carbohydrate malabsorption plays a significant role in IAP, and I agree. But as I researched this issue I couldn’t help asking: what might be causing the carbohydrate malabsorption in the first place, and are there any other causes of bacterial overgrowth that may precede carbohydrate malabsorption? I believe the one answer to both of those questions is low stomach acid. Low stomach acid can contribute to both bacterial overgrowth (independently of carbohydrate intake) and carbohydrate malabsorption, as I describe below. In a nutshell, the process looks like this: Let’s look at each step in turn.
1. Low Stomach Acid Causes Bacterial Overgrowth
As I explain in the next article, one of the chief roles of stomach acid is to inhibit bacterial overgrowth. At a pH of 3 or less (the normal pH of the stomach), most bacteria can’t survive for more than 15 minutes. But when stomach acid is insufficient and the pH of the stomach rises above 5, bacteria begin to thrive. The gastrin knockout mouse, which is incapable of producing stomach acid, suffers from bacterial overgrowth—as well as inflammation, damage and precancerous polyps in its intestines. (4) It is also well documented that acid-suppressing drugs promote bacterial overgrowth. Long-term use of Prilosec, one of the most potent acid suppressing drugs, reduces the secretion of hydrochloric acid (HCL) in the stomach to near zero. In one trial, 30 people with GERD were treated with a high dose of Prilosec (40g/day) for at least 3 months. (5) Eleven of the 30 Prilosec-treated people had developed significant bacterial overgrowth, compared with only one of the 10 people in the control group.
2. Low Stomach Acid Causes Maldigestion of Carbohydrates
Stomach acid (HCL) supports the digestion and absorption of carbohydrates by stimulating the release of pancreatic enzymes into the small intestine. If the pH of the stomach is too high (due to insufficient stomach acid), the pancreatic enzymes will not be secreted and the carbohydrates will not be broken down properly.
Like what you’re reading? Get my free newsletter, recipes, eBooks, product recommendations, and more!
Bacterial Overgrowth + Maldigested Carbohydrates = GAS!
In Hearburn Cured, Dr. Robillard points out that though microbes are able to metabolize proteins and even fats, their preferred energy source is carbohydrate. The fermentation of carbohydrates that haven’t been digested properly produces gas. The resulting gas increases intra-abdominal pressure, which is the driving force behind acid reflux and GERD. From Dr. Robillard’s book:
According to Suarez and Levitt (17), 30 g of carbohydrate that escapes absorption in a day could produce more than 10,000 mL (ten liters) of hydrogen gas. That is a huge amount of gas!
When stomach acid is sufficient and carbohydrates are consumed in moderation, they are properly broken down into glucose and rapidly absorbed in the small intestine before they can be fermented by microbes. However, if stomach acid is insufficient and/or carbohydrates are consumed in excess, some of the carbs will escape absorption and become available for intestinal microbes to ferment.
Other Supporting Evidence
Dr. Robillard also argues that if gas produced by microbial fermentation of carbohydrates causes acid reflux, we might expect that reflux could be treated by either:
- Reducing bacterial overgrowth, or
- Reducing carbohydrate intake.
He points to two studies which demonstrate this. In a study by Pehl, administration of erythromycin (an antibiotic) significantly decreased esophageal reflux. (6)
In another study by Pennathur, erythromycin strengthened the defective lower esophageal sphincter in patients with acid reflux. (7) To my knowledge, there have only been two small trials performed to test the effects of carbohydrate restriction on GERD. Both had positive results. A small case series showed a significant, almost immediate resolution of GERD symptoms in obese individuals initiating a very-low-carb diet. (8) A more recent study found that a very low-carb diet decreased distal esophagus acid exposure and improved the symptoms of GERD. (9) Perhaps most importantly, the magnitude of the improvement was similar to what has been reported with treatment with proton-pump inhibitors (acid suppressing drugs).
Some researchers now believe that Irritable Bowel Syndrome (IBS) is caused by small intestinal bacterial overgrowth (SIBO). (10) A study performed at the GI Motility Center in Los Angeles in 2002 found that 71 percent of GERD patients tested positive for IBS—double the percentage seen in non-GERD patients being examined. (11) The high prevalence of IBS in GERD patients combined with the recognition that bacterial overgrowth causes IBS is yet another line of evidence suggesting that bacterial overgrowth is also a causative factor in GERD.
Final Comments
To summarize, low stomach acid contributes to bacterial overgrowth in the bowel which in turn can lead to carbohydrate malabsorption (due to decreased pancreatic enzyme secretion). Malabsorption of carbohydrates, as Dr. Robillard has pointed out, increases intra-abdominal pressure and causes GERD.
Where Dr. Robillard and I differ is that I believe low stomach acid is the primary problem with GERD, with carbohydrate malabsorption playing a secondary role. I do think that improper digestion of proteins can, in fact, lead to GERD, whereas Dr. Robillard states in his book that putrefaction of proteins is more likely to cause flatulence. This may be so in most cases, but I’ve seen several patients in my practice on very-low-carbohydrate diets who still experience heartburn, which improves upon restoring proper stomach acid secretion (which we covered in another article in this series). In the Part III of the series I discuss the connection between GERD and H. pylori, and further evidence supporting the theory that GERD is caused by bacterial overgrowth. Read on!
Better supplementation. Fewer supplements.
Close the nutrient gap to feel and perform your best.
A daily stack of supplements designed to meet your most critical needs.



My LES nerve was cut when they took a tumor off my spine. I wish I would have known about diet more back then. Perhaps I would not have a hiatal hernia and LPR.
What is you opinion on digestive enzymes containing hydro chlorique acid? Will this help gerd?
Yoga might help in GERD. Has helped me at times!
https://www.ijoy.org.in/article.asp?issn=0973-6131;year=2013;volume=6;issue=2;spage=131;epage=133;aulast=Kaswala
I have also suffered with GERD for years. I started noticing that on days that I had meals high in carbohydrate I would have horrible symptoms sometimes lasting for days. I tried just really cutting back on carbs and there is a huge difference in my health with and without carbs. Protein does not seems to upset my stomach unless the protein also has a lot of fat. I teach anatomy & physiology so I have been experimenting with my diet to find what makes me feel most healthy. I just want to feel good and not be afraid to eat.
Hey I’ve been burping constantly for nearly a year now also had acid reflux couldn’t find the problem until this morning I figured out I couldn’t hold my breath for more than 10seconds..all you have to do to stop the burping is to breath properly in and out of your nostrils and take big deep breaths suck your stomach into your rib cage and hold it for a few seconds until you feel better do this laying on your back do not breath through your mouth cause than you swallow more air and it causes more burping…just relax and take big deep breaths for 2-3 minutes and you will see all the air come out..I thought I had some disease lol, just wanted to share cause I know the feeling and I feel amazing now and also trying eating and drinking slowly ??
You should look into hiatal hernia. That would likely be the cause both issues you’re having. A good chiropractor can adjust you and fix it (don’t go to a modern med doc or they’ll cut you open). Also you can look up self massage to fix hiatal hernia on the web and see lots of videos.
Are you a doctor?
Mick mate where the hell was ya when i was 17 now 27 it took me 8yrs to fined something that worked for me if i dont do similer breathing methods gerd will come back.. doctors told me to give up take this take that feeding me full of sh#t i did not need.. THIS BREATHING THING NEEDS TO GET OUT THERE MATE… G.E.R.D= took alot of enjoible things from me not jst food and health but to evan having a good time with mates. YEARS past doctor after doctor still random vomiting belching cramping and alot more syntems and discomfets… i serched for answers for years i gave up on evrything and i mean evrything i hit the drugs and found myself smoking crack!! I found that after getting high i wasnt sick …. i knew meth is no answer to anything BUT i worked out simple breathing tasks evan streching WORKS BETTER THAN ANY (PHARM) DRUG or (STREET) DRUG.
anyway mate if we could make this common knowlage with younger people evan if helps 1 kid not to make the mistakes i did or for them to go about there day without the anxiety, embarrassment, pain evan sleep problems would be unexpretionalebly gradifying (sorry for bad spelling)
Amen!
Ive had chronic acid reflux for 25 years and maybe ate 60,000 plus acid indigestion tablets(calcium carbonate ones) over the time and now I’m 50. I decided to stop my carb intake. Its gone. Yes, gone. Ive even lost weight. No acid relieve tablets for 6 months. Nothing. I do miss bread though. I can eat as much protein as I like and it makes no difference. No acid attack. Hooray.
Good job. How does a person cut carbs and stay vegitarian? I stopped eating meat about 4 months ago.
Pamela- you probably should just start by eliminating wheat. You might not have to worry about all carbohydrate foods. But if you need to eliminate grains: fruit, veg, beans, nuts, seeds, nutritional yeast have plenty of protein. If you are not vegan, you can also eat dairy and eggs (I don’t, am allergic to both). You can even get vegan protein powders now. I like Lifetime’s Plant Protein unsweetened vanilla (a blend of pea protein, rice protein, hemp seed, and chia seed with the amino acid profile of egg, although I only use it occasionally). There are vegan bottled protein drinks also, some based on soymilk (like Svelte) and some non-soy.
I track all my food (there are plenty of free food trackers today, I use LoseIt on my phone although I don’t care about calories, just protein and fiber). No problem at all getting plenty of protein on a simple vegan diet, even without wheat. My minimum daily target for my size is 40 grams protein but it’s easy to go way beyond that.
You might find you can eat other grains, you might try millet and rice. Barley has gluten in it but you might not be sensitive to it. Wild rice and quinoa and buckwheat also can be used like grains. You can try corn and sorghum (milo) also as well as oats. Amaranth and teff are also good. You can make easy flatbreads out of anything that you can make into a batter, including beans or quinoa or anything. Check on YouTube for videos showing exactly how to do it. You can also make crackers out of any flour: mix with enough water (oil and salt optional) to make a golf ball-sized ball when rolled between your palms, flatten the ball, and either bake or use a tortilla iron. Non-gluten grains won’t stretch like wheat, so rolling them out can be a pain, but you can just flatten enough between your hands. Rolled oats can be whizzed up in a blender to make a flour.
You could eliminate all grains for a couple of weeks and if that solves your problem, just slowly add small amounts of the other grains and grain-like foods into your diet to see if any of them are a problem. You can rotate foods (different grains each day), that can sometimes help.
I can eat small amounts of wheat as long as I don’t eat it every day or at every meal. The best approach for me is the equivalent of one slice of bread or at most two. Otherwise I get persistent painful heartburn that goes on for many hours. Wheat-free products don’t affect me. But every person is different so you need to experiment.
I am 31 years old male, i have been suffering from severe heartburn for 12 years or more now, and i have tried everything, medications, decrease my food intake, till the point i have undergone a Gastroscope a few moths ago, and took medication for H Pylori …. Nothing worked.
Till i stopped eating bread, it happened by a chance of trying on a new diet to lose weight, then suddenly heartburn stopped, then everytime i eat bread it comes back again …. now sometimes it hits me even when i dont eat bread, but at least now i can stay for days without feeling that a hellfire has started in my chest.
Hi. I found that cutting out gluten helped my GERD, but I get GERD when i am hungry…if i dont eat every few hours. Can this still be due to under production of stomach acid, or someother reason? Thx!
It is the same for me; heartburn when hungry.
Again, look into hiatal hernia!
I am a 22 year old girl who’s been dealing with on/off heartburn/acid reflux. The first time I experienced heart burn, I was 17 and it went away after 2-3 weeks (I took no medicine). It didn’t come back until I was 19 and the doctor prescribed 150mg Zantac. I took it twice a day and within a week, it went away. It didn’t come back until I was 21 but this time it was much worse. Zantac wasn’t helping so I took Nexium for 2 weeks. It only helped when I was on the medication. I went off and the heartburn/acid reflux came again. Then randomly, my symptoms cleared up. I still couldn’t have acidic foods (tomatoes, ketchup, vinegar, alcohol), but I could eat other foods again. Then all of sudden, my symptoms flared up about a month ago. I have tried to increase my alkaline intake, eat smaller portions, exercise, and tried homeopathic remedies. They help for a little bit, but not completely. I’m not overweight; I’m actually underweight, I don’t drink, and I don’t smoke. I am scheduled for an endoscopy next week and plan to increase my probiotic intake as well. I self-diagnosed myself with lactose intolerance after exhibiting symptoms that resembled it. I am getting desperate to figure out what the problem is and living with GERD has actually resulted in depression.
My symptoms include: heartburn (with occasional reflux), excessive gas and bloating, frequent chest pain.
Your not alone. Let me know what the best solution is for you.
do you drink coffee?
Did you figure out wat was wrong yet
Anyone found a solution? I am so depressed with this that doesn’t go away, even fallowing a especial diet ?
My son has a bacterial overgrowth and reflux and constipation. He is on a low FODMAP diet and probiotics. (Suggested by his GI specialist) he sometimes has to take an antibiotic called Flagl to decrease the overgrowth, which helps but doesn’t last long. The diet Is making a big difference for him. It focuses on eliminating high fermenting carbohydrates.
Monash university have the leading science and information on the diet. Google them along with Low FODMAP diet
I hope this might help you too
Looks like you have histamine intolerance! Google it. You should avoid histamine-rich food. Ketotifen might help.
mix 70℅ unfiltered apple cider vinegar 30℅ water into a vodka size shooter and drink it. Works like a clock every time.
I asked mybDoc If I could take ACV he saud no…. It woukd be yo harsh on my stonach. What can I do?
Wow….so many young sufferers of heartburn,GASTRITIS,GORD. I’m in my 60 s .Have had these problems for decades. Take Medium. But it doesn’t always work. Yes hunger =heartburn. Yogurt and probiotics are good. Recently had Nurofen for bad Sinus headache. It’s really messed up my gut. Constant burping,diarrhea. I’m making my own sauerkraut,as fermented food is known to help gut bacteria. I wish my fellow sufferers relief from this awful health problem.
I’m very confused. I have been diagnosed with LPR – symptoms: intermittent hoarseness and a sore throat. No reflux or heartburn. Tests: only a laryngoscopy showing redness.
I have an autoimmune disease pemphigus vulgaris and I have had blistering in my throat from this. Healing healing pemphigus sores in my mouth and body look red.
Since 2012 I have taken courses of treatment for PV twice. The first treatment was prednisolone at 30 mg with azathioprine and omeprazole 20 mg. The prednisolone was tapered over 18 months. At the start of treatment I had terrible stomach pain daily which eventually settled and then recurred at various times during and after the taper. I stayed on the omeprazole after stopping the pred for a while but had problems with my stomach as my body had to recover from the after effects of the meds.
My second course of treatment has been for 7 months and I am now on a maintenance dose of steroids and omeprazole (no azathioprine this time). I have had some stomach problems again when tapering.
Before diagnosis of PV I had an investigation by my GP into an intermittent clicking sound when breathing in at night. Whilst we didn’t get to the bottom of it, the tests (barium swallow and a nasal tube to look at my vocal cords) showed no acid reflux but a pharyngeal pouch, slow peristalsys and a hiatal hernia. I realise all of these may predispose me to some kind of acid reflux.
Am I experiencing the throat problems because of reflux due to acid diet/obesity or due to the effects of 25 months of steroids? My diet is pretty well balanced and I never/rarely eat many of the banned substances in the Koufman diet. Or is the problem caused by PV blisters?
How can I get proper answers?
Hello Sue,
I was facing the problem of hoarseness and soar-throat for quite a long time (more than 18 months to be precise). Initially, doctor suggested different medicines for throat infection; nothing worked. After 18 months, I tried proton pump inhibitor, and it really worked. However, I started facing severe indigestion problem after that. And after 6 months or so, hoarseness again re-surfaced.
For me, it seems acid-reflux is the most probable reason for hoarseness. So, yes, It can be a reason for your throat problems.
My son was born with a rare genetic syndrome and one of the main charrcteristic of it is gerd we saw the struggle from almost 1 month of birth server refluxing we landed in the hospital with dehydration from not drinking bottles… He was put on meds like Zantac and Prilosec and reglan for mobility and reflux. I mean we where having multiple episodes of refluxing and spitting up everything. He couldnt be moved at all. We where told the same thing that the sphincter was under developed and that this could be a issues we will deal with on occasion for a while. The meds have kept him comfortable but I’d really like to know what we can do long term besides a Nissian fundoplication. He hasn’t been refluxing much but there’s always the possibility of silent reflux. Just very scary I don’t want him on these meds for a long period of time I need a better resolution.
Gisel,
I am not in the medical field but survived StG IV BrCa 23 years ago by making good decisions.
I wanted to get off Omeprazole 40mg taken daily and still having monthly attacks. I started a “RenewLife, Ultimate FLORA probiotic” from Whole Foods which has 150 billion bacteria, 40 strains. I tapered off the meds and continue the probiotic with great results.
I would ask a medical professional and a pharmacist if trying the probiotic could harm your child…and then try it.
A high acidic diet was the cause of my reflux. Not low acid. So what now?
I think you might have histamine intolerance. Check it up.
I was diagnosed with achalasia. I’ve had laproscopic surgery to help my sphincter muscle to open up. Also, my esophagus muscles that push food down don’t work. So, thanks to gravity it goes down. I usually take Zantac 150 and it helps mostly. I haven’t been lately and seem to be having an orange spit that looks and feels like grease. It’s come out my nose before while I was asleep. Scary! SO. what do u suggest?
Read the article above and give it a try.
For 8 years, every time I got a cold, I had a cough that was completely resistant to ANY cough medicine. Nothing worked on the coughs…..in the last 2 years the cough would appear without having a cold…..then the cough became more of a gagging cough, sometimes vomiting, dry heaving, hacking…..went to doc to be told “you have post nasal drip” I was prescribed a nasal spray….didn’t do anything. Then was told I have airway spasms (though I have no trouble breathing). I was given 2 inhalers including albuterol. Nothing. Doc said “You may have acid reflux” I told her I thought she was crazy. I NEVER get heartburn! Not even when I was pregnant! Went for an upper GI series and saw the reflux with my own 2 eyes. Started 20 mg of Prilosec. Worked like a charm! No coughing fits for about 3 weeks, then it seemed to stop working. Now I’m on 40mg a day and I had a slight improvement. Now I still take 40mg a day but still cough , hack, vomit and dry heave on and off all day long. I am so afraid to stop taking it at this point. its so bad while taking it, I can’t imagine how awful its gonna be off-meds! I DO have quite a sweet tooth and I love pasta, potatoes and all things carb-related…..I am so glad I saw this article! First thing tomorrow I’m cutting out most of my sugar and carb intake in hopes of helping…..I’m desperate! Anyone else have a cough only experience?
Hi Julie,
About 10 years ago I had the same experience with my throat. I was also diagnosed with GERD and Barrets due to a Hiatal hernia. I was in Nerium 40mg and after reading about the side effects I opted for acid reflux surgery which worked for about 6 years. I am bow having the BARRX treatment to get rid of the barrets so I am on PPI again until it’s over (4 treatments over 8 months)
I will follow the recommendations in this article as it makes a lot of sense.It’s about managing the condition.
Hope you are feeling better by now
Rainer
I also heard that KEFIR works for a lot of people.
That is interesting to read all this. I have had a chronic cough that is more than a month long. I had just recovered from the cough a month prior to that lasted 3 weeks then had a period of rest and now it picked right back up and there is no signs of improving. I thought I may have GERD, but was not sure. I was recently diagnosed with CSID or disaccharide intolerance and it has affected me greatly because of sugars and carbs. I have been doing better avoiding it, but my cough is still persistent and it drives me nuts. It is embarrassing too at work because I can’t control it and people are on the phones and here I am coughing my lungs away. I am going to do the suggestion of Hydrochloric acid and see if this helps. No cough medicine or anything helps it –in fact it makes it worse! Because it has sugar in it…
YES!!
I can occasionally have a cough that is so violent I can wet my pants. Gross but true.
My wise doctor suggested I had reactive asthma fixed by using an inhaler. It worked. Turns out if I was exposed to a fragrance I could have this reaction. This just started in the last few years and never happened before, I am over 50. It didn’t matter if I liked the odor or not, some things just set me off. The inhaler that I only use as needed is ProAir.
Good luck!
I used to only have the cough, like you. Especially when I’d bend over, head low, to pick something up, for example. I’d stand up and have that dry cough. Freaked me out! Heart burn once in a blue moon after a big meal but nothing terrible or consistent. Like every 6 months. However, recently I’ve had massive heartburn that lasted about a week straight. I finally put together that the cough and heartburn were both related to acid reflux. Got chest pressure as well (I’m a healthy 48 year old in good shape, eat well, not overweight, exercise regularly…and no cardiac issues. Had that checked when the cough started). Interestingly, I used to follow a paleo diet (which shuns grain carbs) and didn’t experience any of this. Over the past year or so, I’ve moved away from that. Over the past 2 months, I’ve begun using sweetened coffee creamer. I really wonder if these junky carbs have caused the problem!
I have the same problem with coughing …..help please.
My GERD was so bad that I was spitting up all night. What finally worked … Going vegan. My carbs are much higher now but a plant-based vegan diet cured my GERD in a week. I spent years suffering and feel like a new person cutting out all the animal meat and fat, dairy, sugar. It’s amazing.
ugh, I hear ya on the spitting up! I gag, vomit, heave….everything! Is your new diet still helping??? I’m willing to try anything at this point.
Thanks
Julie
Turns out I have a hiatal hernia, which could be the cause. I’m on vegan diet and 80 mg Prilosec. No problems at night anymore.
I’m vegan also however it’s not helped my gerd. What do I do???
About a week after my GERD went away, it came back. I did a barium swallow and found out I have a hiatal hernia, which can cause GERD. I go to the doc on Thursday but in the meantime I upped my Prilosec to 80mg a day. That is high, but it is a dose that can be prescribed. The GERD is gone, like totally gone on that dose, but my doc may want to fix the hernia instead of keeping me on so much Prilosec. I think long term Prilosec can mess with the kidneys.
I’m not vegan, but cutting out caffeine (all sources- coffee, tea, chocolate) and cutting out gluten has helped immensely. The caffeine loosens the sphincter and the gluten causes bloating- a painful combination. Read up on the affects of caffeine.
I am a vegan too and it has helped so much! What do you eat?
That is so weird. I tried to eat a vegan diet and ended up with heartburn (I’m not generally prone to it). It was all the legumes I was eating. Every time I had beans, etc., I’d get heartburn.
Awesome ! Glad it worked! I am vegan 5 years now but still suffer – started probiotics and its a little better – next ill try ACV – seitan / wheat seems to exacerbate it – So glad your trying vegan
I’m vegan and I’m experiencing Gerd symptoms for about 3 weeks now. I’m so nauseous and have headaches, it feels like I have reflux all the time…I had blood work done and everything is fine.
I’m going crazy trying to understand why I’m feeling like this! I eat a lot of carbs, but that’s it. Don’t drink, don’t smoke, don’t eat dairy, etc…
I will try to cut off carbs, I guess I can only eat salads?
Hello,
Thanks for this amazing article. Here is my story.
In Jan 2016 I was diagnosed with Flu and was given antibiotic – Tamiflu. Though it killed off my flu, I started feeling burning sensation behind my sternum after a couple of days. It usually happened after I took meals. As days passed I felt tremendous chest pain similar to some cardiac disease. It made me very nervous.
After visiting my doctor, he prescribed me Somac 40 MG tablet. Relief was immediate & after 4-5 days I felt I was all okay. I stopped taking Somac & later realized that it was a big mistake. My GERD returned with vengeance & there was no option but to keep medication on.
After few weeks I checked with my doctor and he prescribed me Nexium 40 MG. For over a week I started feeling normal and stopped taking medicine in the hope that I’d finally recovered but within 2 days my GERD returned again & with more vengeance. I then realized that my problem lied somewhere else.
After going through number of articles on the internet I found this and though of giving it a try.
Started taking apple cider vinegar prior to meals and for last 3 days I have not had any return symptom of GERD. Also I eliminated carbs and sugar from my diet altoghether & it seems like working. I will get back to normal diet after a week or so.
God bless you all !!!
Hi Suhel,
May I know how is it now. After returning back to normal diet, do you still get GERD?
Hello Fatin,
I am perfectly alright now. I have not had any single episode of GERD for over 2 weeks. Now I have started taking normal diet including meat and carbs.
I had some bowel movement problems for a couple of days but now everything seems so normal.
God bless you all 🙂
Eating acidic food has given me heartburn and regurgitation. Does anyone undergo the same thing as me? In this article, it says that we need more acid to combat GERD. How can I do so if acid is giving me theses uncomfortable symptoms? Help, anyone?
Suhel,
Does taking acidic food (like apple cider vinegar) not cause GERD symptoms for you? How did you cope with it? Please help me on this!
Hello LSTN,
Apple Cider Vinegar helped me a lot. It ultimately turned out that my GERD was actually because of side effect of antibiotics. I have more or less recovered now, have not taken ACV for last 3 weeks, all appears to be okay now.
ACV is indeed acidic but it is less acidic than HCL therefore it makes stomach content less acidic, just right for digestion to take place normally.
Hi Suhel
How much ACV did you take each time before meals?
I have been diagnosed with acid reflux which is really only causing me pain in the throat when I swallow. Thought I’d give ACV a go before starting Nexium 40mg.
Sheila
Hello Sheila,
I have stopped taking ACV altogether. Fortunately I have overcome this condition of GERD.
I suggest you take 1 tbl spoon ACV with a medium sized glass of water.
Since you are facing only throat pain, suggest you to switch to non-acidic diet and see. That should fix it.
Hi Suhel
Thank you for your reply. Just one more question, does it matter what type of ACV I take? I bought an organic one but it is not cloudy so is obviously filtered. Have been on it for 5 days now no real improvement but no worse either. Will continue until I use the bottle up anyway.
Many thanks Sheila
Can you give me an update on the ACV that you tried? I am having the same sore throat caused by acid reflux but no other symptoms.
Can anyone offer advice for belching? I don’t think I have GERD, but for the past 5 yrs I have bouts of belching a couple of times a day, lasting for 10-20 minutes. I suppose I could be swallowing air, but I am not aware of it if I am.
I have recently started taking probiotics to help with bloating, and overall intestinal health improvement, but I am not finding that I have severe heart burn and increased bloating and gas. I am unable to find any info on the internet about probiotics causing this so I am wondering if you may have some insight on this topic. I have never had heart burn prior to this last 10 days. I have recently (in the past 6 months) increased my carbohydrate intake as I am now vegan…wondering if this plus the probiotics are causing the problems?
I just started taking a probiotic for about 6 days and my acid reflux has been so bad while I’m sleeping I feel like I should stop.
Are you taking a soil based pro biotic or one with dairy? If you have a milk allergy or lactose intolerance that may be the cause.
If low stomach acid is really the problem for GERD, how do you get the proper amount of stomach acid? Alcoholic beverages really give me bad GERD.
Try taking apple cider vinegar (unfiltered) prior to meals. See the results for a week or so.
If not then you can consult your doctor and take some HCL tablets.
I have been on meds for acid reflux for a couple of years now and they told me my sphincter doesn’t close properly. I still have many problems with bad gas and diarrhea and don’t know what to do. I take probiotics (have tried several different kinds) and eat fermented cabbage and have tried supplements for the gut to no avail. Any suggestions?!
An HCL supplement. Do an internet search on it and you’ll find all about it and finding the right dose for you.
Have you been tested for Celiac disease and/or lactose intolerance? I had severe GERD, a hiatal hernia, constant gas, and other stomach/intestinal problems attributed to IBS. Turns out I had both Celiac disease and lactose intolerance that presented in some unusual ways (hence not being tested despite years of these problems). Once gluten and dairy were eliminated from my diet, I immediately stopped having ANY reflux or stomach problems. If you’re not able to be tested right away, try eliminating grains (all wheat, barley, rye, oats, etc.) and dairy (including butter) from your diet for a few days and see what happens. A drastic diet change can be a difficult adjustment, but if it works, it’s worth it. Good luck!
I suffered with heart burn/refux for the past 30 years, all the different meds out there I have been on sometimes more than one at a time. Nothing stopped it completely. I stopped taking meds a year ago and tried the home remedy thing , baking soda, apple cider vinegar etc all worked but not completely. 2 weeks ago I decided to try no carbs in an effort to lose some mid life weight and I have not had a single episode of either heart burn or reflux since the second day of no carbs, let me be specific, I don’t eat any flour, sugar, bread, potato, and other starchy veg, and I limit all fruit except for berries right now. It made me so mad that no one ever said hey try no carbs it might help or I would have done this years ago. It still freaks me out to eat and have no digestive issues. I am always waiting for it to kick in but so far nothing!!!! It’s a miracle to me that it’s was one or all of the carbs that was causing my issues. I am a definite believer and will pass this on to anyone e who listens in the hope of helping others like me who have been on it all. I take a multivitamin and a daily probiotic and I am going to look at taking digestive enzymes also just to help heal my poor stomach.
Hi Anne,
Nice to hear good change in you. Even I have been struggling with reflux for past 6 years. Does stopping carbohydrate really help you? Kindly share . I am desperately looking for some relief inspite of being on Nexium. Thanks
So you eat a low-carb diet? I am too skinny to go to such lengths. I’m trying to gain weight not lose it. I need to eat food that will bulk me up. I don’t process proteins well and personally am not crazy about meat. If I give up carbs altogether and only eat protein in moderation you’d wouldn’t be able to see me sideways. There has to be a better alternative than to just stop eating starchy carbs.
In low carb diet one substitutes carb calories with fat. And protein intake stays as per your metabolic requirement.
Please tell me the foods I could eat to get rid of this awful reflux …and….gain weight. Thank you.
It’s not the low carb that cures it. Carbs are energy and energy can’t hurt anyone at all. In going low carb one manages to also avoid lots of starch. Lo-carb diets avoid starchy foods because they turn into sugar and that is not good for dieters because it makes them put on weight. Starch is the enemy here. Dr. Sebi always says that starch is bad for the body for the most part. so avoid the foods that are high in starch and you’ll most likely be healthier in general alongside chilling your acid reflux
Very interesting George. I’ve heard of Sebi, and was getting into him but many of the foods seems to make the symptoms worse. Chickpeas, fruit, tomatoes, mushrooms, seem to agitate the acid in a way. I prefer vegan but I think meat gives me less issues. Small amounts and no carbs. Help if you can.
Hi I am also having gerd . Tried all medics but now I got somthing which is drinking pomegranate juice in empty stomach really hepled me out …
Anne I’m definitely going to try your strategy in hopes of it working for me I haven’t felt well in years like 8 years so desperate for a solution.
I had excately the same experience. When I went low carb to loose weight the symptoms disappeared, but the minute I started eating carbs again the symptoms were back. I love carbs
So what does your diet look like then. I want to try this to get rid of my sore throat from acid reflux. Thank you!
I started losing my voice over the summer, and attributed it to sleeping near the air conditioning unit at first. When I saw my doctor, we tried some allergy meds and it didn’t work. After a serious of multiple visits and about 7-8 different doctors (and even a steroid/ hormone test since I am a weight lifting woman), I finally got an appointment with ENT.
Before I even had the camera down my throat, they said I had GERD. When they looked for sure, they’re convinced. However, I experience zero heart burn or normal symptoms of acid reflux. I do have a higher protein intake, and clean carbs, but I eat well and have cut things out. I also have stopped taking pre workouts and it’s now been 3 months since my diagnosis and my voice still isn’t normal. Will I ever get my voice back? I used to sing and I miss it. Anyone else experience this symptom?
Something like this happened to my aunt. They are still trying to figure out the cause, some of her doctors think it’s caused by Lyme disease
vocal cord dysfunction happens after having GERD.
One good exercise that i do, is using a empty lollipop stick, the white ones with a hole on it. Put it in your mouth and blow it making a sound of ambulance with your vocal cords, WIIII-UUUU-WIIIII-UUUU.
Also working on breathing properly.
Try a homeopath specialist or consult aherbalist.or naturopath
I went through exactly the same problem as you . I ended up with throat cancer from gerd. Stage 4a, to be exact. The chemo and radiation nearly killed me. My voice is back to normal now except when my gerd is really bad . I get scoped annually. They want to do surgery to narrow my esophagus. Nope. I don’t eat much as it is. Rarely carbs. Going on the apple cider vinegar thing. My gerd ebded up so bad that i wake up cjoming in the night, bloat every time i eat have ibs now, lost five molars yo scid teflux. This life has been hell for 7 years. I wish i woukd have believed them ehen they said reflux the fitrst yime my vouce went south…
I’ve lost my voice on several occasions and noticed comments of me having a raspy voice however I’ve never had one before unless sick. I have a raspy voice now n usually do more raspy than not. I would like some advice on that if anyone would like to share.
I have the same symptoms of horseless, loosing my voice and I feel I have mucus stuck in my throat. I was told by my Dr that I have Gerd with LPR (silent reflux)
She did a test on my that measured my Ph level over 24 hours. I was a 17 level. She put me on a two week diet where I ate only food over a ph5 and only drank smart water which is water with a high ph. I drink trader joes and Evamor which are over ph8 level. When I went back my acid level,was down to a 10. She wants it at a 9. I am taking PPI in the morning and Zantac 150 before lunch and dinner and befor bedtime along with gavison advanced before bedtime to protect my esphogus. (The meds are temporary)
This Dr has help several oprea singers and is a well know Dr and author in this field. I go back on Tuesday and I am hoping she starts to Wien me off my meds.
Hi Susan, can you please tell me the name of your doctor and the book she wrote? I have similar problems for the last 2 months and have changed my diet and still no improvement. I’m going to try a different PPI today (the last one didn’t work at all).
My Dr name is Dr Jamie Kaufman and she is in Manhatten. The name of her book is Dropping Acid the reflux diet and cure.
How is your voice today?
Yes my voice went a few weeks ago. Reflux and cough…not flu. Throat sore. Used to sing too. No joy. Nexium is a daily take for me. When I wrote my previous comment nexium came up as medium. Correction now. M D